By Sujith Kumar Prankumar, Gurjeet Kaur, Samitha Fernando and P. Arun Kumar
At 20, Eugene* was a military serviceman and medal-winning sportsman. Tall, charismatic and intelligent, he was living the life of his dreams and feeling invincible. But one day, he suspected he may have acquired HIV after developing flu-like symptoms. Not long before that, he'd had unprotected anal sex. Eugene was apprehensive at first about taking an HIV test, but after talking to his best friend he decided to put aside his anxieties and get tested.
To his immense relief, the results came back negative.![]()
![]()
Image via rawpixel.
A decade since that fateful day, Eugene can still recall the thoughts that raced through his mind. “ I didn’t want to go at first,” he shared, in an interview. “For me, AIDS was the worst thing that could happen, and I’d rather die than find out that I was HIV positive. On the other hand, if I didn’t take the test, I could just pretend everything was okay.”
Eugene’s initial response is telling of a deep-seated stigma and lack of awareness about HIV and AIDS. For one, he clearly did not know the difference between HIV and AIDS, the latter being the disease resulting at a late-stage from untreated HIV infection. Neither was he aware that medicine has advanced to a point where contracting HIV is no longer a “death sentence”. With the appropriate treatment, persons with HIV can expect to have a normal lifespan and would not be able to pass the virus to anyone else if they maintained an undetectable viral load. Furthermore, there is Pre-Exposure Prophylaxis (PrEP) for individuals at high risk of HIV. PrEP is an HIV prevention method in which people who don't have HIV take HIV medicine daily to reduce their risk of getting HIV if they are exposed to them.
Eugene additionally presumed that HIV-related treatment would be costly, risky and ineffective—and that his medical records would be shared with the government, future employers, and even his family. Had his best friend not persuaded him to get tested, all of these pre-conceived notions about HIV would have prevented Eugene from taking that crucial first step.
Pooja,* 45, worked long days as a primary school teacher. When she came home, she was caregiver to her mother who had Alzheimer’s disease. In this most common form of dementia, the brain is progressively damaged, and one’s memory and judgement become impaired.
![]()
![]()
Image via rawpixel.
Pooja’s mother behaved erratically towards the end of her life: she was often emotionally volatile and had difficulty remembering things. Caregiving took a personal toll on Pooja: while she did her utmost to see to her mother's needs, inside she felt lonely, resentful and emotionally distant.
Today, 15 years since her mother’s death, Pooja continues to feel regret and guilt about her feelings towards her mother nearing the end of the latter's life. As a teacher, she often taught her students about filial piety and the importance of caring for one’s parents and the elderly. But at home, she felt a disconnect from what she preached.
Besides being incurable, HIV and dementia share something else in common: they are both socially and historically stigmatised conditions that can have long-lasting and deleterious effects on individuals and their communities.
Although neither Eugene nor Pooja had HIV or dementia, they experienced immense feelings of stress and shame. These emotions—compounded with a lack of awareness—discouraged them from accessing much-needed care for themselves.
Stigma, Oppression, Bias: What’s In a Name?
Stigma refers to the phenomenon in which an attribute or community is discredited and marginalised due to societal bias. Oppression relates to actions that result from stigma and bias. Bias describes conscious or unconscious negative or prejudicial attitudes that affect behaviour—it can be damaging to the well-being and self-esteem of marginalised individuals and communities.
Broadly speaking, stigma presents a barrier to prevention and care: despite advances in medical science, it prevents individuals and families from accessing essential information and interventions that could dramatically improve their quality of life.
Effects of Stigma: HIV
When it comes to HIV, stigma and discrimination can take many forms, including travel bans and visa restrictions, excommunication from families and communities, being barred from housing, education, employment and access to health and social services, loss of reputation, harassment and blackmail, legal persecution, and so on. Persons living with HIV—or assumed to be at risk of HIV—are therefore susceptible to harassment, abuse, discrimination, violence, poor mental and physical health, and even homelessness and poverty.
HIV-related stigma can also cause individuals to engage in risky behaviours such as re-using needles and syringes, not getting regularly tested for STIs, and having unprotected sex. Fearing they would be judged, persons with HIV may also be reluctant to be publicly seen at places like clinics, or be afraid of hospitalisation due to previous experiences of discrimination and/or stigma from healthcare professionals. “Double gloving” of medical staff, for example, insinuates that persons living with HIV are “contagious”, even if their viral load is undetectable, or if they’d been hospitalised for other acute conditions.
Frequently Asked Questions: HIV
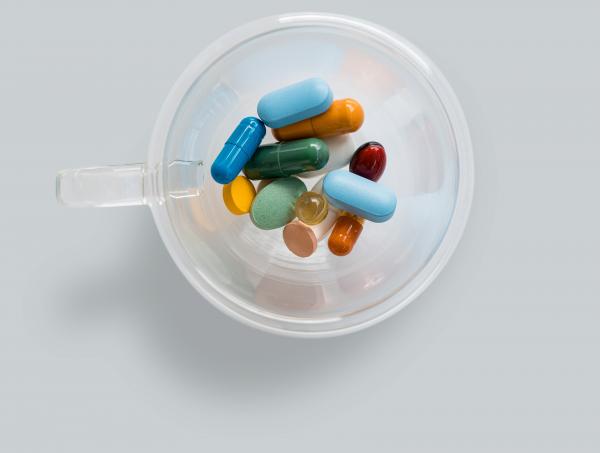
Image via Unsplash.
Does HIV = AIDS?
No, this is a central misconception. HIV refers to the human immune deficiency virus infection whereas AIDS, which stands for acquired immune deficiency syndrome, is the advanced disease stage of HIV infection. AIDS can develop as a result of not receiving proper medication during the early stage of infection.
Is HIV a death sentence?
Thanks to advancements in novel medications, HIV is no longer a death sentence. These drugs not only help improve the immune system of patients, but also inhibit HIV replication. For the past few decades, the medications have significantly improved the longevity and quality of life of persons with HIV—many of them can expect to lead active and healthy lives like anyone without HIV.
If both partners have HIV, do they still need to worry about having unprotected sex?
Yes. Someone living with HIV can get re-infected with a different strain of HIV. If this strain of HIV is more resistant to the current treatment, that will dampen the efficacy of treatment and cause immune suppression.
With the novel medications in HIV, should we no longer worry about getting it?
While currently available medication can effectively suppress HIV, there is no known cure. Similar to any other drugs, HIV antiretroviral therapy has side effects that are yet to be fully evaluated. Moreover, people living with HIV have a higher risk of developing certain cancers and other infections if the disease is not well controlled. Hence, prevention is key.
Can HIV be spread by touching, living together or sharing food?
No. HIV is transmitted via certain body fluids, namely blood, seminal fluid, pre-ejaculate fluid, vaginal fluid, anal mucous and breastmilk. More specifically, it is spread during unprotected sex, pregnancy, childbirth and breastfeeding, blood transfusions, organ transplants and the sharing of needles and syringes.
Effects of Stigma: Dementia
Persons with dementia similarly experience discrimination and feel disempowered by the stigma and bias surrounding their condition. This fear of being judged or perceived differently may even keep some from seeking early diagnosis and assessment.
However, unlike HIV, there is currently no treatment to reverse or impede the onset or progression of dementia. As such, it remains a challenge to maintain dementia patients’ safety in hospitals and to keep them as active as possible. Tending to persons with dementia additionally calls for high levels of care, placing immense physical and emotion strain on their families and caregivers—sometimes even past the patient’s death, as we saw in Pooja’s case.
Thankfully, we are starting to see some successful efforts around the world to mitigate the stigma relating to HIV and dementia.
Frequently Asked Questions: Dementia
![]()
Image via rawpixel.
What is normal brain ageing?
There are some normal, age-related changes like difficulty with multitasking and slower processing speed, but routine memory and knowledge do not get affected much. It is normal to forget recent events like the name of the person you met today and where you parked your car.
What is not normal brain ageing?
Severe memory loss that interferes with your daily life is not part of the normal brain ageing process. Common symptoms of dementia include difficulty recognising close friends and family members, frequently misplacing regular-use items, taking much longer to complete normal tasks, inability to find one’s own house, and confusion over the function of items.
Can young people get dementia?
Yes. Many people believe that dementia is a normal part of old age, but this is unfortunately not the case. Early-onset Alzheimer’s disease (the most common form of dementia) among persons aged 30 between 65 years accounts for 5 to 10 per cent of all Alzheimer’s disease cases.
Can dementia kill you?
Dementia is a group of conditions or consequences of many diseases with definite symptoms, including Alzheimer’s disease and Parkinson’s disease. Alzheimer’s, for example, is a progressive brain disease in which brain cells lose their connections, degenerate and die, which can be fatal since the brain is responsible for the body to function.
Is early diagnosis of dementia helpful?
Although there is no cure to reverse or treat dementia once the disease has damaged the brain cells and disrupted the important functioning of brain, early diagnosis provides the opportunity to learn and understand the condition of patients. Finding out early empowers patients and their families with more time to choose the appropriate treatment, and make diet and lifestyle adjustments.
Global Efforts: HIV Stigma Mitigation
Australia’s public health response to the HIV epidemic is a result of strong grassroots activism and engagement with government, health professionals and “affected” communities, based on the principle of harm reduction. Harm reduction, or harm minimisation, is aimed at reducing negative social and medical consequences of engaging in legal or illegal behaviour such as drug use and sex work. Some of its activities include needle and syringe exchange and drug treatment programmes, peer education and the provision of condoms and lubricant. The country has also been at the forefront of ensuring its people of access to treatment and information. PrEP, the aforementioned HIV-prevention method, is now subsidised by the Australian government.
At the other end of the globe, Brazil has, for decades, adopted a human rights-based approach towards tackling HIV. Not only does the Brazilian government offer education programmes on prevention strategies, it also provides free and universal access to antiretroviral medication, treatment and self-testing kits—in partnership with marginalised communities, civil society, medical professionals and researchers. These efforts have dramatically reduced AIDS-related mortality and hospitalisation rates in the country. Brazil has additionally lowered prices of HIV medications globally by challenging pharmaceutical companies and producing generic versions; to date, its government is the world’s largest buyer and distributor of condoms.
Five Ways to Support People Living with HIV

Image via Unsplash.
1. Educate the Public
Lack of knowledge and enduring myths about HIV have resulted in a great deal of stigma experienced by persons living with HIV, to the detriment of patients and their families. Therefore, educating the public on facts about HIV is absolutely critical to reduce the social burden of those who live with HIV.
2. Educate the Affected
There are numerous services available to help persons living with HIV to improve their quality of life. These include professional counselling services and professional advice relating to work and lifestyle adjustments.
3. Extend Your Support
Almost every person diagnosed with HIV will go through massive psychological stress due to societal pressure and its reputation for being an incurable disease. Create a friendly environment where they can access support, but give persons with HIV the time and space to feel comfortable about coming forward and opening up. Meanwhile, establish a good rapport when you are in the conversation. Be aware of the language you use and make sure that you make them feel empowered.
4. Be Respectful
If someone reveals their HIV status (or serostatus) to you, respect their privacy and the fact that they chose you as their listener. They opened up about their HIV status because they trusted you. Hence, disclosing their status to others without their permission is immoral. If you breach this trust, they may not trust anyone again. Respect their rights as fellow human beings.
5. Seek Treatment Early
There are a few key elements in the medical management of HIV infection. For example, the earlier the treatment starts, the better the prognosis will be. Hence, seeking medical advice following the diagnosis is essential. For many, starting treatment can be a daunting experience. This fear can delay treatment, which can lead to HIV-related health complications. After starting on medical treatment, compliance with the medication is of utmost importance. Adherence to the regimen of medication will stop the progression of the disease by hampering virus replication and preventing the risk of developing AIDS. It is important to know about the risk associated with poor compliance to treatment, and how the virus can build up resistance against the treatment, resulting in a more aggressive disease.
Global Efforts: Dementia Stigma Mitigation
Recognising that existing treatments in standard ageing care are limited when it comes to dementia—and the benefits that come with staying active—the Netherlands launched the world’s first dementia village in 2009. At Hogeweyk, a community-care facility located in Weesp, use of the social-relational concept reduces the stigma typically tied to dementia and living in an aged care home. Residents of Hogeweyk lead full and independent lives, with access to amenities including a salon, cinema, café, pub, town square and supermarket. They have also been found to live longer, eat healthier, be less medicated and to feel happier.

 Image via Flickr (CC BY-NC-SA 2.0).
Image via Flickr (CC BY-NC-SA 2.0).
Inspired by Hogeweyk, other countries have announced versions of model environments for their dementia communities. In Singapore, where nearly three in four persons living with dementia feel “rejected”, its government announced plans to build its first dementia care village in Sembawang. And over in Australia, where dementia is cited as a National Health Priority Area, construction of the country’s first dementia village is underway in Tasmania.
Five Ways to Support People and Families Living with Dementia


Image via Unsplash.
1. Plan activities
It is very important for people with dementia to engage in meaningful and enjoyable activities. Support from friends and family to achieve social contact, skills and pleasure will boost their self-esteem and sense of empowerment.
2. Ensure a safe physical environment
People with dementia experience difficulties with coordination and visual observation. It is thus crucial to prepare a safe working area with minimal distractions and noise. Pay attention to surroundings, such as the presence of furniture, sharp objects, cleaning chemicals, or anything that is potentially hazardous.
3. Don’t give up
Proper knowledge and awareness are very important for people with dementia, as well as their family, friends and caregivers. Caring for someone with dementia is physically and emotional challenging because they can behave aggressively, hallucinate and have sudden mood changes. Understand that this is not anyone’s fault. Rather, be understanding of any behaviour fluctuations and avoid making the other party feel like a failure or burden. Further, do not undertake caregiving all by yourself—find a support system to relieve you where necessary, and carve out personal time to see to your own well-being, too.
4. Don’t feel embarrassed
Persons with dementia often feel isolated because they feel embarrassed by their behaviour, or because they believe their loved ones are embarrassed by them. If you or someone you love has dementia, tell people around you about the disease so as to destigmatise the condition.
5. Make necessary legal and financial decisions
The ability to make accurate financial and legal decisions decreases as dementia progresses, so if you’ve received a dementia diagnosis, make future plans as early as possible. Contact your lawyer or manager to make necessary arrangements and manage your money if needed. Contact your local dementia care centre for legal advice and to understand your options.
Challenges Ahead
Whether we're talking about HIV or dementia, much remains to be done in the fight against stigma, oppression and bias.
As of 2019, there has been a decline in new HIV cases in Singapore, but the stigma remains pervasive. In Australia, though HIV rates are also falling, it is increasing among Asian-born men, a large group of whom are international students. Carrying with them internalised stigma that discourages them from accessing the health and educational resources, few are aware of their rights and responsibilities. Meanwhile in Brazil, after the election of a new populist government led by President Jair Bolsonaro, an illiberal nationalist with known homophobic views, there is genuine concern over the possibility of the reversal of evidence-based policies in favour of a hard-line and religiously conservative approach that could negatively impact the HIV epidemic.

Image via Pexels.
As regards dementia, many societies the world over continue to view the condition as a natural process of ageing instead of the chronic disease that it is. An overwhelming majority of people also believe they will eventually be diagnosed with the condition themselves, while those living with dementia try to hide it out of fear that their opinions would not be taken seriously or that they would be treated unfairly in healthcare, social, or home settings. Without a cure at present, it is ever more important to combat stigma with more awareness about the disease, and by encouraging understanding and empathy towards persons with dementia.
In conclusion, stigma and discrimination are social processes that can be undone with the right mix of political and social will. We can reduce feelings of isolation and shame, and break down barriers to care by building more aware, compassionate and inclusive societies. Supported by structural solutions such as stronger public education, anti-discrimination laws, multi-sectoral partnerships, subsidised treatment costs and preventive treatment, we can destigmatise deeply personal conditions like HIV and dementia.
Today, Eugene is more aware about how to deal with HIV risk. He describes how differently he’d handle a HIV-positive diagnosis these days compared to ten years ago: “I’d still be scared about my employer and family finding out, but at least now I know there is effective treatment available. I’ll take comfort knowing I won’t die from it and that I have friends who love me.”
As for Pooja, she balances any guilt she continues to feel with a deeper sense of empathy for caregivers of persons with dementia—having personally been down that road. She also feels optimistic about greater opportunities to support the dementia community and their caregivers. “There wasn’t as much awareness or discussion of dementia back in the day,” she says. “Currently there are TV programmes about it and I even see informational leaflets at clinics. Things are better now.”
*Editor’s Note: Names have been changed for privacy.
Banner image: Photo by mentatdgt via Pexels
  |
Sujith Kumar Prankumar is a Scientia PhD scholar at the Centre for Social Research in Health, UNSW Sydney, where he is investigating ethnicity, sexuality and belonging. His research interests lie primarily in social medicine, identity and well-being. Sujith holds an MA (Human Rights Studies) from Columbia University and an MTS (Women, Gender, Sexuality and Religion) from Harvard University, and has worked in higher education, social innovation, media, development and inclusion in Boston, Singapore and Sydney. He can be reached at sujith.kumar@student.unsw.edu.au |
  |
Gurjeet Kaur is a Scientia PhD scholar at the Centre for Healthy Brain Aging, UNSW Sydney, where she is investigating new therapeutic drug target biomarkers for early diagnosis of a rare form of dementia called Autosomal Dominant Alzheimer’s Disease. Prior to her PhD studies, Gurjeet was a research fellow at the National Dairy Research Institute and received her MSc in Biotechnology (Molecular Biology and Proteomics) from Thapar University, India. Gurjeet can be reached at g.virk@student.unsw.edu.au |
  |
Samitha Fernando is a Scientia PhD scholar at the Faculty of Medicine, UNSW Sydney. A medical doctor with a special interest in infectious diseases and Immunology, Samitha obtained his MBBS and MPhil (Immunology) from the University of Sri Jayewardenepura, Sri Lanka. His doctoral research investigates the roles and regulation of immune responses to infectious diseases such as Dengue, Zika, West Nile and Influenza virus infections. His main objective is to develop novel therapeutic strategies to improve patient care by better understanding the pathogenesis of infectious diseases. Samitha can be reached at b.fernando@student.unsw.edu.au |
  |
P. Arun Kumar is the Programme Executive for the National HIV Programme, at the National Centre for Infectious Diseases, Singapore. He is a registered nurse with an MPH (Health Promotion and Disease Prevention) from the University of Queensland and a BSc (Nursing Practice) from the University of Manchester and the Singapore Institute of Technology. Arun has over seven years’ experience in HIV, sexual health, community engagement and programme management, and has spent over three years conducting HIV social research with culturally diverse populations nationally. In this time, he has conceptualised community-informed health promotion campaigns on HIV testing and treatment, and implemented social support programmes to promote healthy living among marginalised populations. Arun can be reached at arunkumar0990@outlook.com |







Comments